Robert Sobukwe Hospital Respond to Concerns
Statement from Robert Sobukwe Hospital in response to concerns raised on social media by Tumelo Mosikare
DATE: 26 January 2019 9:18AM
MEDIA STATEMENT START
We are aware of the concerns being raised on social media and the local newspapers over the past few days about patients seen lying on the floor. We wish to give further information and insight into this situation.
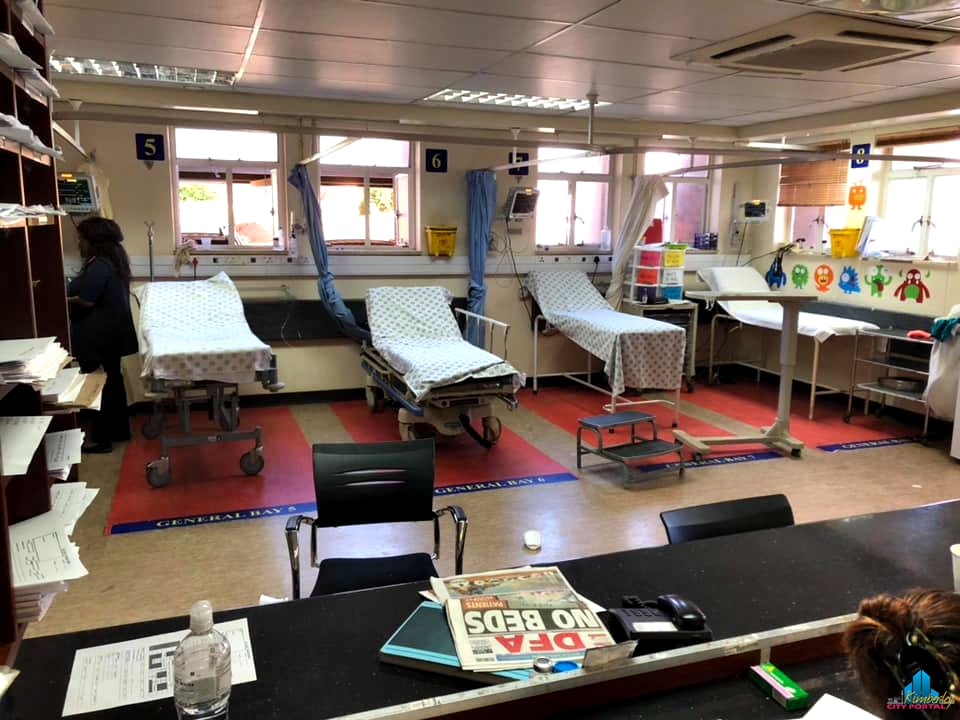
The patients shown in the photograph are not waiting to be seen. All of these patients have been triaged by a nurse and doctor and then admitted to the Emergency Centre (EC) for observation and/or treatment of their psychotic behaviours.
These patients have been admitted because they were presenting with psychotic behavior and require observation for their mental health condition. They have been given medication to help manage their behaviours. They are awaiting transfer to the mental health assessment ward which at that time was full with 18 patients (13 of these were waiting for beds to become available at the mental health hospital). We are hopeful that the new mental health hospital will provide a solution to this. Most of these patients had either a bed, trolley or chair available to them but chose to lie on the floor.
It was commented in the media that one or two patients had a drip inserted. When patients are admitted to EC we always insert a drip line in case medication needs to be given quickly.
Another was said to have an oxygen mask. The patient sitting against the wall at the back was not a mental health patient but a patient being administered oxygen for breathing problems (COPD). He was sat in the chair which is next to him but he chose to sit on the floor and lean against the wall.
On the left and the right of the photo are two relatives sitting in chairs, the one on the left is seen waving to the camera.
In terms of the mental health patients lying on the floor. When this photo on social media was taken there were some beds available – on the extreme left of the photo an empty bed can be seen. There were also some empty trolleys available as well as chairs.
We have included a second photograph which was taken the same time but on the next day (Friday). This shows the trolleys directly opposite the area where the mental health patients are located. It aims to show that whilst the mental health patient situation opposite is similar, on this side of the room there are available trolleys for patients in the Emergency Centre.
We don’t want to underplay the issue of high influx of mental health patients who first have to be assessed in a general hospital before possible referral to the mental health hospital.
However, we often find that the mentally ill patient will choose to sit, lie and walk about. They are a challenging group of patients to manage in the emergency centre, and indeed should not normally be kept in the Emergency Centre. But on occasions the numbers are so great that we have no choice. This is when the staff may push the beds and furniture to one side and create the open space as shown in the photograph.
===============
Now let us turn to the patients waiting in the A&E waiting area in front of the admissions counters. As we have said, none of the patients in the photograph are waiting in this area to be seen by a doctor or nurses.
We are well aware of many patients who wait a long time in A&E. These are nearly always patients who have been triaged as “green” (routine). In an ideal world these patients should not have self referred to Robert Managaliso Sobukwe Hospital A&E. In an ideal world they would refer themselves the previous day or the next day to their GP or primary health care clinic.
Our policy of never turning a patient away means that these “green” patients can sometimes wait many many hours before being seen by the doctor and discharged for a minor condition.
We recognize that many patients don’t have a lot of choices or don’t know what choices are available to them. Relatives are often scared for their loved ones and want reassurance. We are not making excuses as to why we may find relatives or patients lying across the benches in the waiting area, we are just trying to explain some of the complexities.
Patients are seen in Accident and Emergency according to clinical priority and their clinical urgency.
The South African Triage System is used where patients are colour coded in terms of clinical urgency.
Patients coded as red are emergency patients and are seen immediately or within 10 minutes. These patients are often brought in by ambulance and taken straight to the Emergency Centre.
Patients coded orange are urgent and are seen within 10 – 60 minutes.
Patients coded as yellow are less urgent and are seen within 4 – 6 hours. In many instances these patients should have gone to their local clinic or pharmacy earlier that day or the next day.
Patients coded as green are routine and will often have to wait in excess of 6 hours. These patients are encouraged to visit their local clinic or pharmacy, but we will never turn a patient away from the hospital.
We are often asked why are the queues so long?
The people waiting to be seen in queues are in most cases not clinically urgent and will wait while more serious cases are attended to first. We thus encourage clients with minor ailments to visit their local clinics. Many of us will know of relatives or friends whose life or limb was saved by receiving rapid treatment at hospital.
Critically ill patients are not made to wait. Clients with a change in condition (worsening) is also fast tracked and seen. We do find that a patient with a broken small bone, for instance, thinks they are an emergency and doesn’t understand why they must wait. But we do have to deal with heart attacks, choking, stabbing to an artery, etc, as more urgent. We also aim to prioritize very small children as their condition can change rapidly.
We are often asked, “When should I visit A&E?”
Firstly, major traumas (stabbing, head injury, broken long bones, etc) will normally be brought in my an ambulance. But if you have a major wound you should always rush to hospital.
But most of our A&E patient volumes are self referrals with medical complaints.
While nobody wants to be a nuisance, here are 5 symptoms (red flag conditions) you should never ignore. In these cases, getting to A&E for a proper check-up and appropriate treatment could be life-saving.
1. Severe chest pains.
Severe, persistent chest pains – which might be felt as a tightness, squeezing or pressing sensation – could indicate a heart attack.
Pain might also travel down the arms (usually the left one), in the jaw, neck, back and abdomen; and other symptoms include breathlessness, sweating, anxiety (often described as ‘a sense of doom’), nausea and vomiting and coughing or wheezing. If you suspect a heart attack, it’s absolutely crucial to call an emergency ambulance and get to A&E immediately.
2. Difficulty breathing.
Shortness of breath that doesn’t feel normal, or that’s causing you to feel unwell or worried, should never be ignored. It might be due to something harmless, it could be an anxiety attack – or it might be an asthma attack, allergic reaction (particularly if accompanied by swelling around the face/mouth area) or due to underlying illness, obstruction or injury. The important thing is to get it thoroughly checked as soon as possible.
3. Slurred speech and droopy face.
As with heart attacks, a suspected stroke should always be treated as an emergency. Stroke symptoms can vary in severity, but don’t take any chances – as if it is a stroke, speedy treatment can mean the difference between life and death, and long-term disability.
Learn the FAST acronym that will help you diagnose a stroke: Face-Arms-Speech-Time. It’s common for the face to droop on one side (the person might not be able to smile or fully open their eye); there may be paralysis in that arm, too; the person’s speech may become slurred or garbled, they might be talking in a confused way that makes no sense, or possibly unable to speak at all. And the ‘T’ stands for ‘Time’: time to call an emergency ambulance.
4. Acute mental confusion.
A sudden confused and disorientated state that’s out of character and causing concern could be due to a number of things. Again, it may be a symptom of a stroke, or it could be as a result of a severe infection (is there also a rash, fever, vomiting?).
It could even be caused by concussion following a knock to the head – which may have happened hours or days previously. Whatever the cause, its best to get things checked as a matter of urgency.
5. Loss of consciousness.
A simple fainting episode – particularly where there’s a clear cause, such as a person has become too hot – is not usually a medical emergency.
But there are exceptions, and any mysterious loss of consciousness, or repeated fainting attacks or seizures, if accompanied by other symptoms or physical trauma – especially if the person’s pulse becomes very weak, erratic or fast – should be treated as a potential emergency. Call for an emergency ambulance if you become worried.
So that’s the top five “red flag conditions”. But there are always exceptions – and sometimes symptoms that feel very severe might turn out to be harmless (for instance, it’s common for people experiencing severe indigestion to fear they’re having a heart attack). Remember that it’s better to be safe than sorry: if you’re worried, get things checked by the experts. It’s far better to feel a little bit embarrassed than risk your health.
Once you’ve been triaged (assessed and prioritized) by the nurse or doctor, you will have to wait your turn. We don’t simply treat people on the basis of first come first served. You will be seen on the basis of your clinical urgency. Someone with a stab to the heart will be treated within seconds, whereas a headache or stomach ache with no other critical symptoms will often have to wait for many hours as more sick patients take preference.
It makes sense – if we are really sick it’s what we would want. If you have a sickness developing over a number of weeks, days or hours, don’t simply wait until the evening, night or weekend to go to A&E. Take precautionary steps during the day and visit your GP, Clinic or Pharmacist to get advice.
MEDIA STATEMENT START
ORIGINAL CONCERN RAISED BY TUMELO MOSIKARE- 24 January 2019 10:33 AM
Robert Sobukwe Hospital this morning..
Patients waiting on the floor for services since last night and having to sleep on the floor
This is not because of Doctors or Nurses… it is because those in charge of the administration of the hospital, the Directors and Managers do not find the need to give our people decent services..
They know their family members and they themselves do not use these public services so why bother to make them of quality
He loa itebala
It was easy to change the name of Hospital to honor a hero of South Africa’s struggle… now this is the dishonour you show him and his people on a daily basis?